News
L.casei Shirota: inflammation and immunity in athletes
Athletes training at a high intensity experience increased incidence of upper respiratory tract infections. The mechanisms responsible for such effects are presumed to be involved with the activation of the inflammatory response. Inflammation is triggered, among others, by mucosal dryness and higher exposition to pollutants influenced by hyperventilation in the upper airways.
A recent study by Vaisberg et al. has found that L.casei Shirota, besides modulating the immune response in the airways, may also regulate the systemic response post-marathon1.
In their randomised placebo controlled trial, 42 male amateur runners consumed either 40 x 109 L.casei Shirota (n=20) or placebo (n=22) 30 days prior to the marathon. The effects were followed by changes in immune/inflammatory parameters in the nasal mucosal and serum, concentrations of secretory IgA and antimicrobial peptides in saliva.

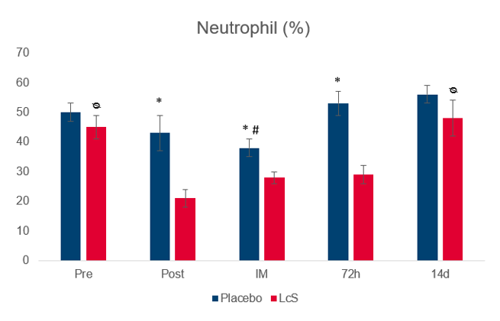
Fig. 1. Neutrophil infiltration in nasal mucosa (%). Pre: before 30 days the competition; Post: 30 days after ingestion and 24 h before the competition; IM: immediately after the competition; 72h: after the competition; 14d: after the competition.
*differences between placebo and LcS group for the same occasion; # differences between IM and Pre, 72 h and 14 d in placebo group; ᴓ differences between Pre or 14 d and Post, and IM and 72 h in LcS group.
Interestingly, both groups presented increased serum levels of IL-1ra, IL-6 and IL-10 immediately after the marathon, suggesting a classical anti-inflammatory state due to exercise, however, IL-10 levels in the L.casei Shirota group were higher. The authors previously hypothesised that an increase in IL-10 may be protective against mucosal inflammation in response to a marathon which might be beneficial to the upper respiratory tract2.
In the study, runners with upper airways symptoms had alterations in IL-6 and IL-10 levels (measured in the upper airways). Furthermore, the IL-10/IL-12 ratio in the nasal mucosa was higher in the L.casei Shirota group than the placebo after the marathon. This ratio has been proposed as a tool to measure the balance between anti- and pro- inflammatory states3.
Alterations of TNF-α and IL-1β are commonly found in acute and chronic airway inflammation4,5. Serum concentrations of TNF-α increased in the placebo group after the marathon. Such elevation was associated with an acute pro-inflammatory status induced by the competition.
Decreased salivary SIgA, LL-37 and lysozyme and defensin-1 and increased proinflammatory cytokine levels were observed in the placebo group. The maintenance in the peptides observed in the L.casei Shirota group may be key in the inhibitory effect of the strain against pathogenic bacteria, as suggested by the authors.
Altogether, these findings show the inflammatory effects on the mucosa and the systemic immune response in marathon runners and how L.casei Shirota can have an impact on positively counteracting these changes.
References
1. Vaisberg et al. (2019) Nutrients 11(7): 1678.
2. Vaisberg et al. (2013) Exerc Immunol Rev 19: 49-59.
3. van Hemert et al. (2010) BMC Microbiol 10: 293.
4. Jayne et al. (2018) Am J Respir Cell Mol Biol 58(3): 310-319.
5. Wei-Xu et al. (2016) Mediators Inflamm 2016: 3128182.
19/02/2020